Are you constantly sneezing, dealing with an itchy nose, watery eyes, or skin rashes with no clear cause? You might be suffering from allergies, and identifying the trigger is the first step to finding real relief. At my ENT and allergy clinic in Delhi, we offer Skin Prick Testing (SPT) – a fast, accurate, and minimally invasive method to diagnose a wide range of allergies.
Skin Prick Testing is a simple and effective diagnostic tool used to identify specific allergens that may be causing your symptoms. It helps pinpoint whether you’re allergic to dust mites, pollen, pet dander, mold, foods, or other environmental triggers.
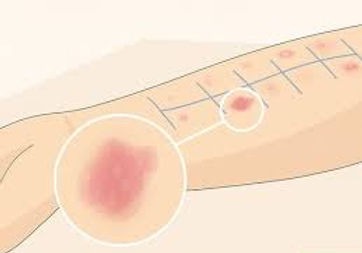
During the test, small amounts of suspected allergens are applied to your skin—usually on the forearm or upper back. A tiny prick or scratch introduces the allergen just below the surface. If you’re allergic, a small, raised bump (similar to a mosquito bite) will appear within 15–20 minutes.
Accurate and immediate results Covers multiple allergens in one session Minimally invasive with no blood draw Safe for adults and children Helps guide personalized treatment plans including allergy avoidance, medication, or immunotherapy (allergy shots).
Skin prick testing is highly recommended if you experience:
Frequent sneezing, nasal congestion, or runny nose (allergic rhinitis)
Chronic cough or asthma symptoms
Itchy or watery eyes
Eczema or unexplained skin rashes
Food-related reactions
Recurrent sinus infections or nasal allergies
Identifying the allergens you react to is essential in managing and preventing flare-ups effectively.
Before coming in for a skin allergy test, you may need to stop taking certain medications (like antihistamines) that can interfere with the results. We’ll provide a full list and guide you through the preparation process.
With over a decade of experience in treating ENT and allergy-related conditions, I provide comprehensive care using evidence-based methods. At our Delhi clinic, we offer:
Accurate skin prick testing using certified allergen extracts
Comfortable environment for adults and children
Personalized treatment plans tailored to your allergy profile
Follow-up care and education for long-term allergy control
Don’t let unidentified allergies affect your comfort and quality of life. Skin prick testing is a fast and reliable way to get the answers you need and start breathing easier. Schedule your allergy evaluation today at our ENT and allergy clinic in Delhi, and take the first step toward a symptom-free life.

Fluid behind the eardrum. Constant ear infections. A child who keeps pulling at their ears or struggling to hear clearly. These aren’t problems you should simply “wait out.”
When the ear cannot drain properly and infections keep returning, a simple but effective procedure called Myringotomy with Grommet Insertion can make a significant difference.
Let’s understand this in a simple and practical way.
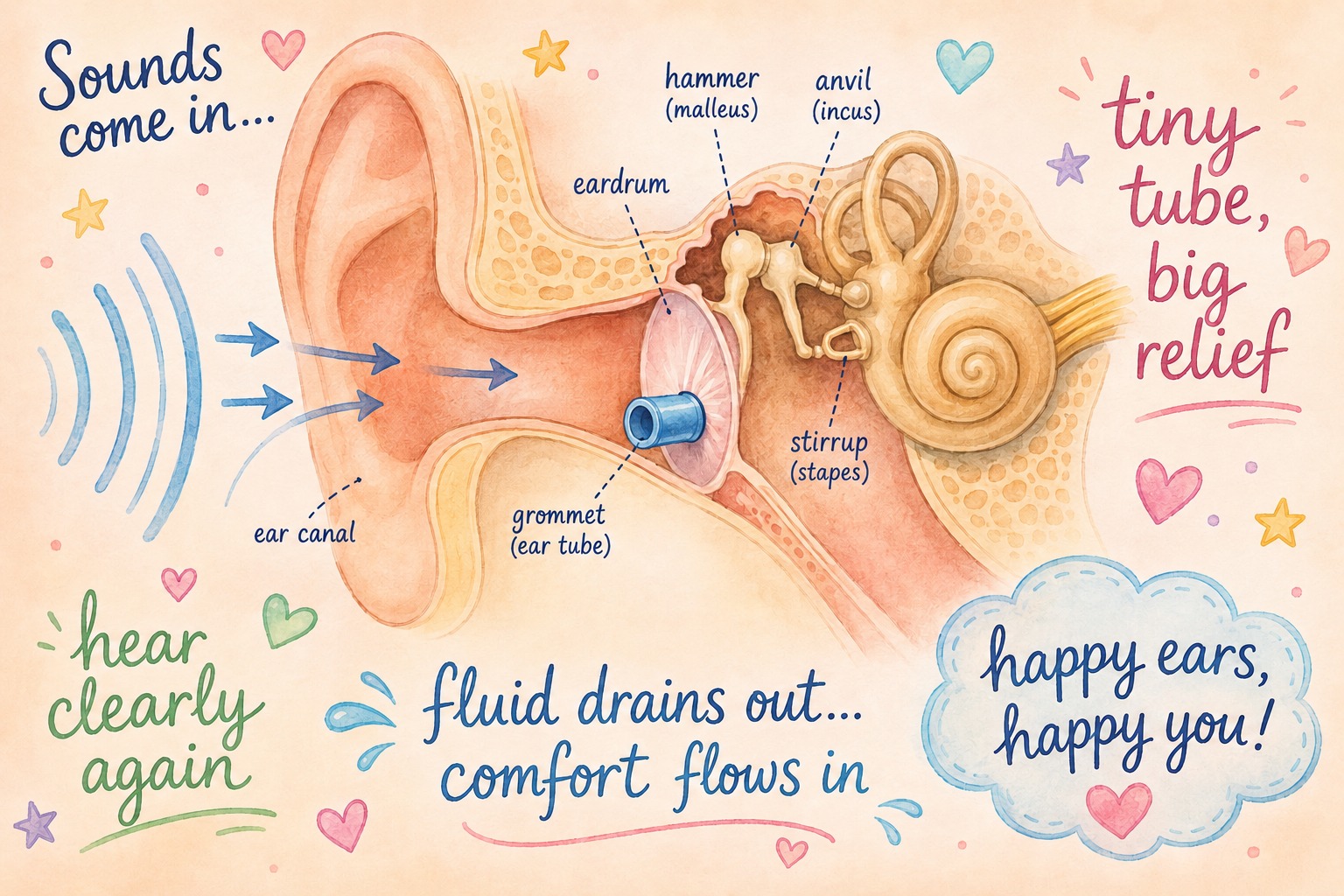
Myringotomy is a minor surgical procedure where a small opening is made in the eardrum to drain fluid trapped behind it.
A Grommet (Ear Tube) is a tiny tube inserted into that opening to keep it open, allowing fluid to drain continuously while maintaining proper airflow inside the middle ear.
Together, these procedures restore normal ear function and significantly reduce recurring ear infections.
Many parents and patients dismiss these symptoms as “just another ear infection,” but repeated episodes often signal an underlying issue.
Not sure if these symptoms apply to you or your child?
The middle ear is connected to the back of the throat through the Eustachian tube. This tube regulates pressure and helps drain fluid from the ear.
When the tube does not function properly, fluid becomes trapped behind the eardrum, creating the perfect environment for infections and hearing problems.
When fluid remains trapped for too long or infections continue recurring, hearing and ear health can both be affected.
Doctors usually begin with medications and monitoring. But surgery becomes the right option when symptoms continue or affect hearing and quality of life.
Myringotomy with Grommet Insertion is considered one of the safest ENT procedures, especially in children. However, like any procedure, certain risks may exist.
No. It is performed under anesthesia, and recovery is generally comfortable.
Most patients notice improvement within days after the fluid drains and airflow is restored.
Usually between 6–18 months before naturally falling out.
Swimming advice may vary depending on the patient. Your ENT specialist will guide you accordingly.
Your ENT specialist will assess whether reinsertion is necessary based on symptoms and fluid buildup.
No. Adults with chronic Eustachian tube dysfunction or recurring fluid buildup may also benefit.
Recurring ear infections and fluid buildup should not be ignored. Early treatment can improve hearing, comfort, and long-term ear health.
Breathing through your nose should feel effortless. But if you’re constantly dealing with blockage, sinus pressure, or difficulty sleeping because of poor airflow, it might not just be a temporary issue.
Conditions like a deviated septum or chronic sinus blockage can affect your daily comfort more than you realize. Procedures like Septoplasty and FESS (Functional Endoscopic Sinus Surgery) are designed to correct these problems and help you breathe better.
Let’s understand this in a simple and practical way.
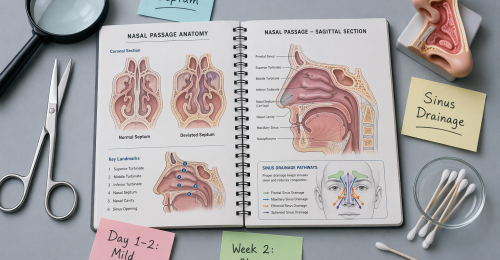
Septoplasty is a procedure that corrects a deviated nasal septum — the thin wall inside your nose that separates both sides. When this wall is not straight, it can block airflow and make breathing difficult.
FESS (Functional Endoscopic Sinus Surgery) is used to open blocked sinuses and restore proper drainage using a small camera (endoscope).
In many patients, both problems exist together. That’s why these procedures are often done together for better, long-term results.
Many people get used to these symptoms and think they’re normal — but they’re not.
Not sure if these symptoms apply to you?
The septum may be off-center from birth or due to injury. When it shifts significantly, it can block airflow and make one nostril feel constantly congested.
Your sinuses need to drain properly. But due to:
…the drainage pathways get blocked, leading to pressure, discomfort, and repeated infections.
When both conditions exist together, symptoms tend to become more persistent.
Not every case needs surgery. Doctors usually start with medications. But if symptoms continue, surgery may be the next step.
Septoplasty and FESS are generally safe, but like any surgery, some risks exist:
No, it is done under anesthesia. Post-surgery discomfort is mild and manageable.
Improvement starts within 2–3 weeks as swelling reduces.
No, septoplasty focuses on breathing, not appearance.
Yes, though sinus care may still be needed.
Get expert evaluation and treatment guidance from an ENT specialist.
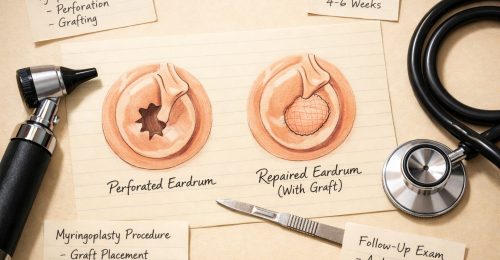
A perforated eardrum a hole or tear in the thin membrane separating your outer and middle ear is more common than many people realise. The good news: most perforations heal on their own, and when they don’t, effective treatments are available.
Consult Dr AashimaLearn More About Treatments
Disclaimer: This article is for general informational purposes only and does not constitute medical advice. Recovery timelines mentioned are typical estimates individual results vary. Always seek guidance from a qualified healthcare professional.
Symptoms depend on the cause, size, and location of the perforation. Some people notice a dramatic onset (such as after a loud blast or ear infection), while others discover the condition gradually.
Not sure if your symptoms match a perforation? A specialist can confirm with a simple ear exam.
The majority of small perforations particularly those caused by infection or minor trauma heal spontaneously within 4 to 8 weeks without any intervention. However, surgery becomes the appropriate path when:
Your ENT surgeon will assess perforation size (often using an otoscope or microscope), hearing test results (audiogram), and overall middle ear health before recommending surgery.
Endoscopic ear surgery has grown significantly in adoption over the past decade. By working entirely through the natural ear canal opening, it avoids the traditional post- auricular (behind-the-ear) incision, which means no visible scar and typically less postoperative discomfort.
However, there are limitations to be aware of:
Important: The “best” technique depends on your individual anatomy, perforation characteristics, and surgeon expertise not one approach suits all patients. Discuss options thoroughly with your ENT.
Wondering if endoscopic surgery is right for you?
Recovery varies depending on whether the perforation healed naturally or required surgery. The timelines below are typical estimates individual experiences differ.
An ENT specialist can confirm your diagnosis, discuss your treatment options, and guide you through the recovery process.